Services
Division of Spine Surgery

Staff
The Division of Spine Surgery at the Department of Orthopaedics and Traumatology, University of Hong Kong has served as a specialist center for Hong Kong Island for many years. The Division is also a tertiary/quaternary referral centre for the entire region and receives referrals from China and Southeast Asia. The Division dedicates its time among Queen Mary Hospital (QMH), Duchess of Kent Children’s Hospital (DKCH), Gleneagles Hospital, Hong Kong Sanatorium & Hospital, The University of Hong Kong Shenzhen Hospital and MacLehose Medical Rehabilitation Centre which is a dedicated centre for spinal cord injury rehabilitation. It enjoys a long history of spine surgery marked by the advent of the anterior approach for the treatment of spinal tuberculosis in the 1950s, which has since been referred to the world over as “The Hong Kong Operation.”
Collaborative approach to care
DKCH is internationally renowned for its care of both pediatric and adult patients. Having once been a major hub in Asia for the treatment of spinal tuberculosis and post-polio deformities, the team currently focuses on patients with scoliosis and other spinal deformities as well as degenerative conditions of the spine.
In 1993 the Center for Spinal Disorders was established and continued collaboration with the Division of Rehabilitation ensures comprehensive, complimentary services for chronic back pain are on offer. This includes assessment, treatment, and rehabilitation which is reliant on a multidisciplinary care team comprised of: the orthopedic surgeon, bioengineer, clinical psychologist, nurse, occupational therapist, pain specialist, physiotherapist, prosthetist, interventional radiologist, and social worker.
First to introduce scoliosis school screening
Working with the Department of Health, the Division was the first to introduce a scoliosis school screening programme in Hong Kong in 1995. Since that time, the program has screened approximately 1 million students, resulting in over 300 yearly detections and referrals to early treatment and prevention of surgery. This is one of the most successful and sustainable programs in the world to date. To further support this program, the division has further implemented measures to improve brace compliance. The vast experience from the above further established the leading role of the division locally, regionally and internationally.
Acute spinal conditions
Queen Mary Hospital carries the dual designations of level one trauma center and university teaching hospital, which means that QMH handles acute conditions, such as spinal fractures, infections and tumors. In addition, an acute spinal cord injuries unit and Center for Paraplegic Walking at the MacLehose Medical Rehabilitation Center round out the division and work to assist patients to maintain mobility. Our recent development of exoskeleton also helps improve mobility of paraplegic spine patients.
Novelty in the past decade
Magnetically controlled growing rod (MCGR) system: To overcome the limitations of traditional growing rods, a remotely distractible, magnetically controlled growing rod (MCGR) system has been developed to allow for gradual, non-invasive spinal lengthening under continuous neurological monitoring in an awake patient on an outpatient setting. The division continues to serve its pioneer role in MCGR and shares our experience with other spine surgeons over the world regularly.
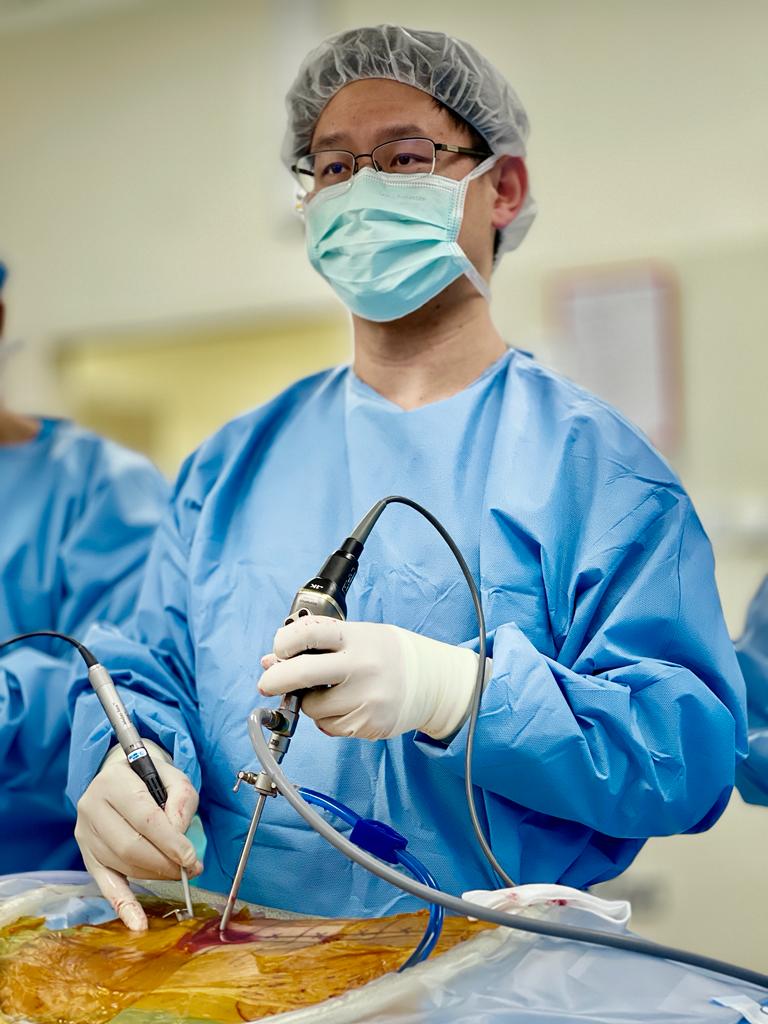
Vertebral Body Tethering (VBT): The division was the first institution to perform this non-fusion surgery for scoliosis in Hong Kong. This technique uses the patient’s growth potential to achieve scoliosis correction while maintaining the patient’s spinal mobility. With the advantages of smaller incisions, smaller wounds, and less postoperative pain, this VBT technique enables faster recovery of patients when compared with conventional spinal fusion treatments.
Spinal cord injury treatment and rehabilitation: The division was the first in Hong Kong to introduce diaphragmatic pacemaker insertion for mechanically-ventilated high-cord injury patients, as well as to utilize powered robotic exoskeletons for early rehabilitation of tetra- and paraplegic patients. The SCI program in QMH and MMRC pioneered clinical service, research, community service, public advocacy and education. In 2020, the SCI team was given the prestigious “Outstanding Team Award” in Hong Kong by the Hospital Authority. Visit www.sci.ortho.hku.hk for details.
Education is paramount
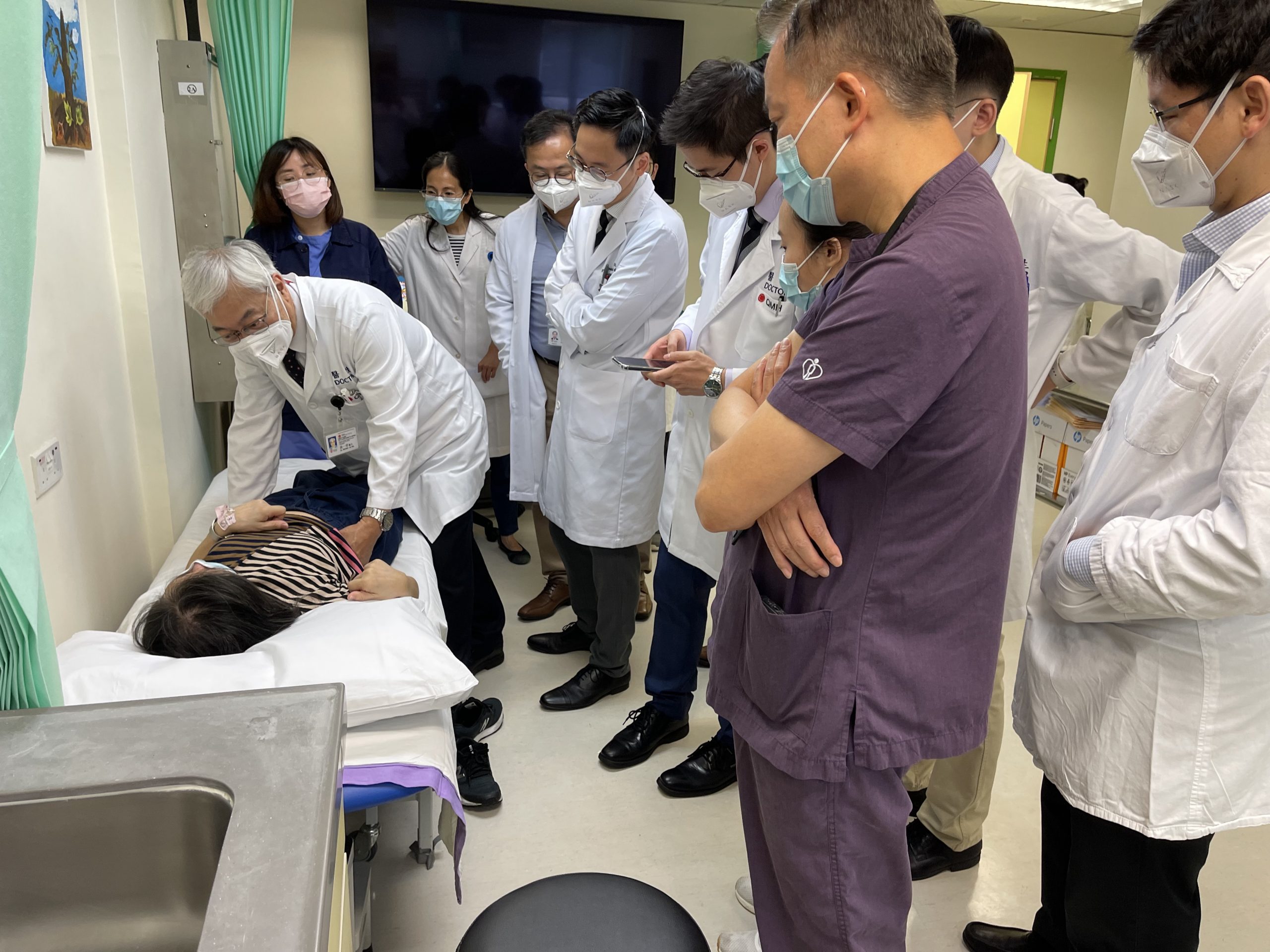
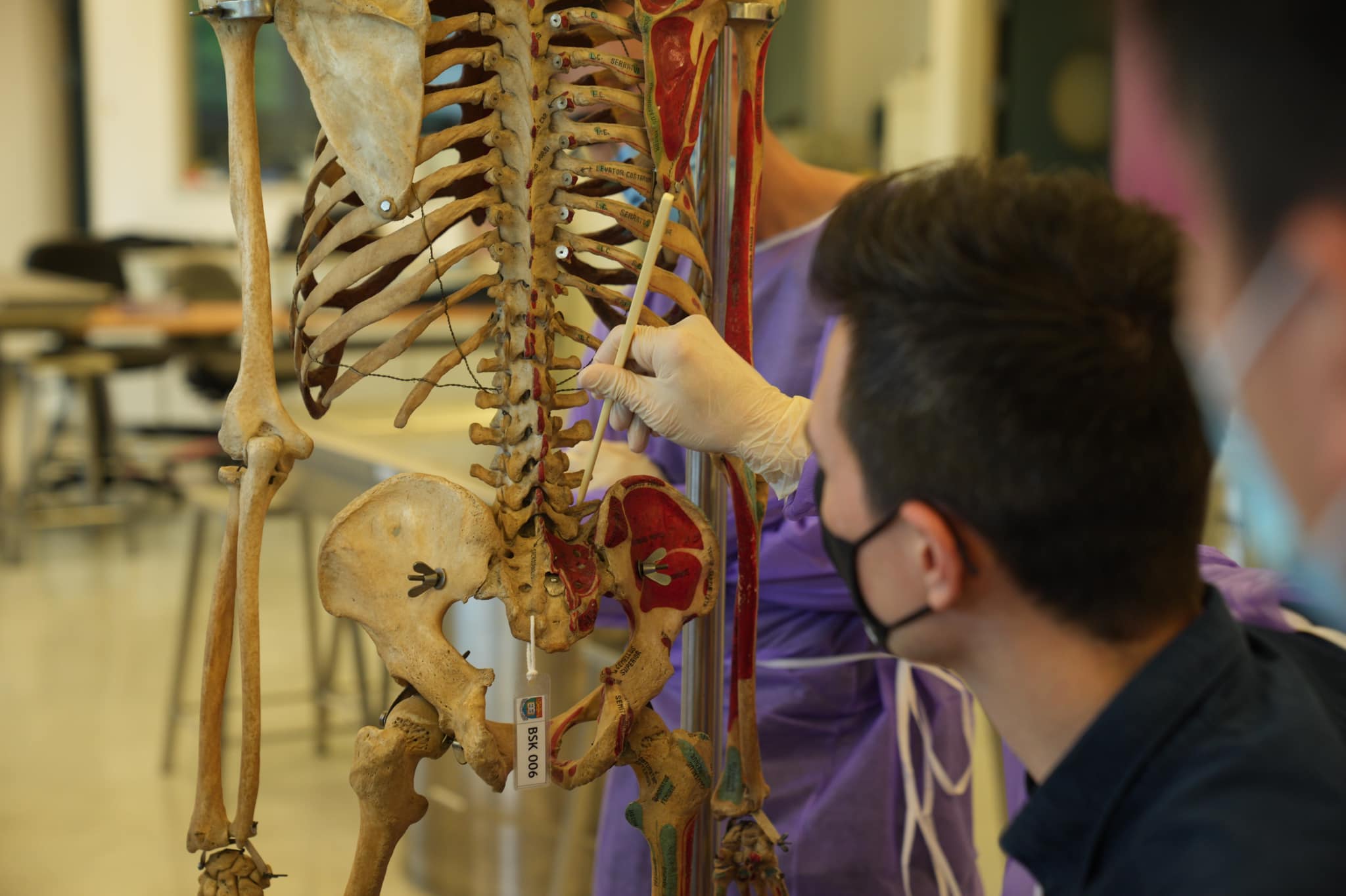
Education, knowledge exchange, and training to improve patient care have always propelled the Division. It offers research and clinical spine fellowships as well as AOSpine sponsored fellowships, which to date has trained over 100 spine surgeons, representing all 7 continents of the globe, that have received training and gone on to operate, teach and pursue research endeavors throughout the world. The hallmark of the Division is in its rational and principled treatment of spinal conditions, based on evidence-based medicine. Fellows visiting the Division are witnessed to the meticulous discussion of each case and the careful consideration of treatment options. Furthermore, the Division has received various Visiting Professors throughout the years to further broaden and exchange knowledge of spinal disorders as well as establish research collaborations.
As an International Spine Reference Center, the Division organizes and hosts international and local training courses and workshops each year, as well as contributing to the research and development of AOSpine, International Society for the Study of the Lumbar Spine (ISSLS), Scoliosis Research Society (SRS), Asia Pacific Spine Society (APSS), International Society of Orthopaedic Surgery and Traumatology (SICOT) programs.
Research of the highest caliber
Well known for modern, novel research and innovation related to spine surgery, the Division has published numerous articles in esteemed international journals that highlight their dedication to advancing the field.
A comprehensive research team supports intensive basic and clinical research into spine-related issues. Current research topics include: genetic epidemiology and molecular mechanisms of intervertebral disc degeneration, intervertebral disc regeneration and tissue engineering, intervertebral disc transplantation, bioactive bone cement, superelastic spinal implants, and surface modification of implants.
Of particular note is the center’s demonstration of the world’s first human disc transplant, which introduced a new research platform investigating allogeneic intervertebral disc transplantation for the treatment of degenerative disc disease. In addition, the spine team has established the largest population-based cohort in the world aimed to identify genetic, environmental, lifestyle, and molecular factors related to disc degeneration and pain. This cohort project entails international collaboration and has received over 15 million USD in funding support, currently supported by a competitive theme-based research grant of Hong Kong.
Another important aspect of the division included the development of the magnetically controlled growing rod (MCGR) system. It had the first MCGR done in the world and pioneered research related to its first clinical trial, distraction methodology, ultrasound radiation-free distraction monitoring and long-term follow-up.
Overall, throughout the years, the clinical and basic science work of the spine team has led to major publications in esteemed journals, such as the Lancet, PNAS, Journal of Human Genetics, Arthritis and Rheumatism, and the Journal of Bone and Joint Surgery, and has received numerous accolades and international awards.
60 years of innovation
1960s
- The “Hong Kong Operation” for spinal tuberculosis (anterior debridement and spinal fusion)
- Transoral approach to the cervical spine
1970s
- The halo-pelvic apparatus
1980s
- Use of a titanium mesh block (one of the earliest forms of cages) for anterior spinal fusion
- Transpedicular decancellation osteotomy for ankylosing spondylitis
1990s
- The fulcrum bending radiograph for scoliosis assessment
- Routine use of intraoperative multimodal spinal cord monitoring
- Initiation of scoliosis schools screening programme in Hong Kong
2000s
- Development of a smart memory shape alloy rod for gradual scoliosis correction
- Gene mutation discovery of scoliosis
- Prone traction radiograph for assessing vertical instability in spondylolisthesis
- Intervertebral disc transplantation
- Biological therapy for disc degeneration
2010s
- Novel superelastic nickel-titanium spinal rod in adolescent idiopathic scoliosis
- Application of magnetic growing rod technology for early-onset scoliosis
- Serum biomarkers of disc degeneration
- New distal radius ulna (DRU) classification for assessing skeletal maturity
- Novel imaging of the intervertebral disc
- Genetic epidemiology of disc degeneration and pain
2020s-present
- Artificial intelligence algorithm for automated deformity assessment
- Automated MRI segmentation
- Scoliosis and osteoarthritis genetics
- Brace outcomes prognostication
- 3D spinal deformity research and EOS imaging
- Proximal femur maturity index for skeletal maturity assessment
- Health-related quality of life research
- Non-fusion surgery for scoliosis: vertebral body tethering
Training opportunities
Link to spine fellowship programme