Services
Division of Joint Replacement Surgery

Staff
The Division of Joint Replacement Surgery is a sub-specialty division under the Department of Orthopaedics and Traumatology, the University of Hong Kong. The Division was founded more than 20 years ago by Professor Kwong Yuen Chiu and now consists of 6 full-time specialist orthopaedic surgeons. Dr. Henry Fu is the current chief of division and Dr. Amy Cheung is the current deputy division chief.
Scope of service
The Division serves as a regional tertiary/quaternary referral centre. The main bulk of clinical services provided by the Division is at Queen Mary Hospital, the flagship teaching hospital of the Faculty of Medicine, University Hong Kong. Elective and emergency operations, in-patient and specialist out-patient clinic services are provided here. Currently, more than 500 joint replacement procedures are performed at Queen Mary Hospital each year.
The Division also operates a Joint Replacement Center under the Hospital Authority at the Duchess of Kent Children’s Hospital where more than 300 joint replacement procedures are performed yearly.
Joint replacement services are also provided by the Division at the University of Hong Kong Shenzhen Hospital, Hong Kong Sanitorium and Hospital and Gleneagles Hospital, with a combined annual volume of around 250 joint replacement procedures. Since January 2019, robotic-arm assisted hip, knee and partial knee replacements have been added to our operating armamentarium.
Research
The Division is at the forefront of arthroplasty research in the region with more than 130 publications in international and local journals thus far and more than 30 podium presentations by our members in local and international academic conferences yearly. The Division is also involved in numerous multi-centre studies based in Asia.
Education
Training offered by the Division has been held in high regard by both international and domestic colleagues. The Division has hosted more than 200 arthroplasty classes with more than 2000 participants and is an accredited Mako Robotic Arm Assisted Joint Replacement training centre.
Highlights over the years
The Division of Joint Replacement Surgery, Department of Orthopaedics and Traumatology, University of Hong Kong was founded by Professor KY Chiu
First to use computer navigation technology in total knee arthroplasty in Hong Kong.
First to use patient specific cutting jigs in total knee arthroplasty in Hong Kong.
Enhanced recovery after surgery (ERAS) practises, were adopted by the Division to optimise patient outcome after surgery. Members of our multidisciplinary team from Queen Mary Hospital have benefitted from the tutelage of Professor Henrik Kehlet and his team.


The Joint Replacement Centre of the Hong Kong West Cluster of the Hospital Authority was established at the Duchess of Kent Children’s Hospital.

Establishment of the Comprehensive Osteoarthritis ManagEment (COME) program, a multidisciplinary, first-of-its-kind exercise program in Hong Kong focussed on the non-operative management of osteoarthritis of the knee.



Establishment of a multi-disciplinary Integrated One-Stop Clinic at the Maclehose Medical Rehabilitation Centre via a donation of 20.7 million HKD from the Hong Kong Jockey Club Charities Trust.


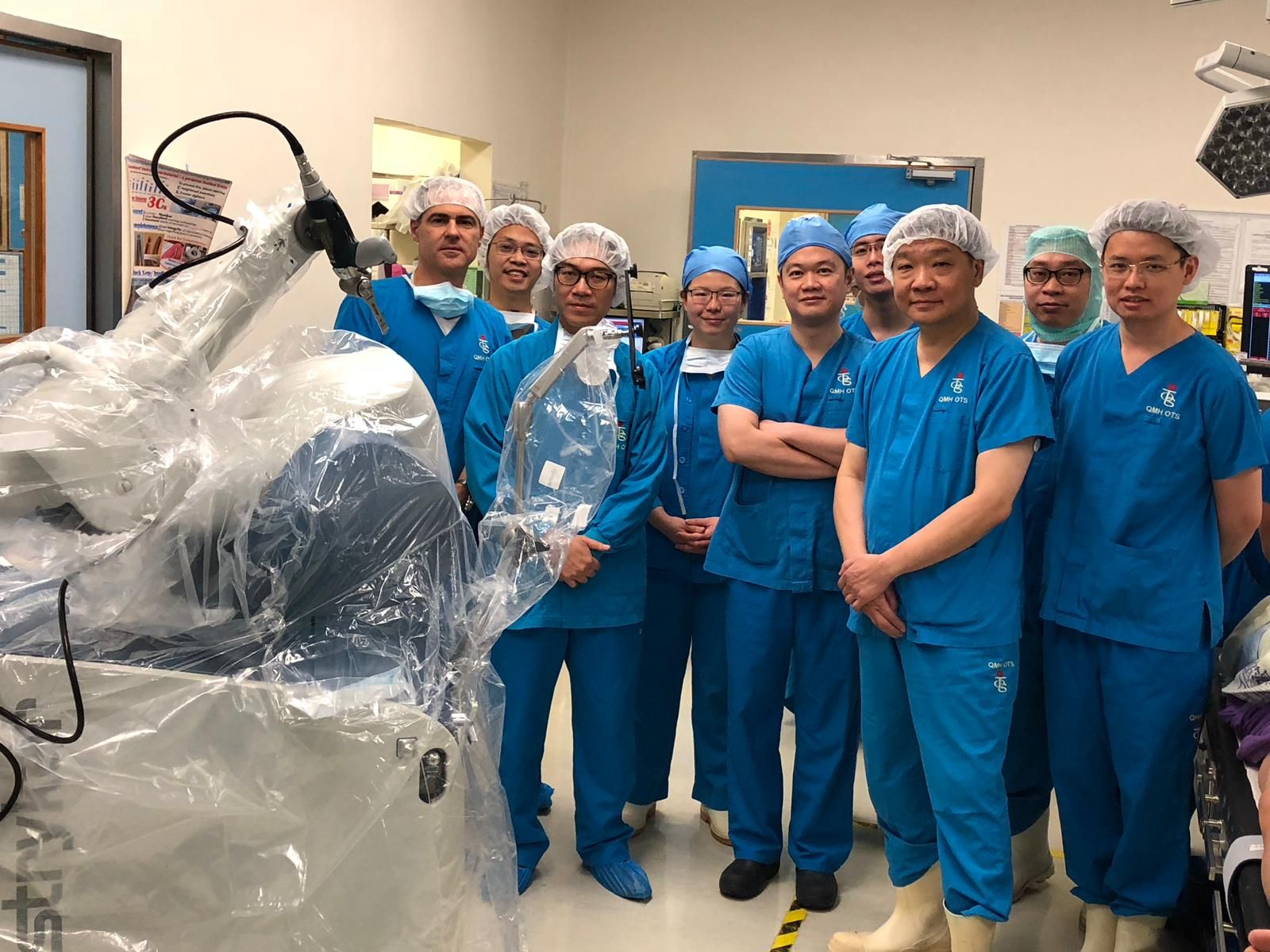
First to perform and promulgate robotic joint replacement surgery in Hong Kong.


Members
Professor KY Chiu, Dr. TP Ng, Dr. WP Yau, Dr. WM Tang

Professor KY Chiu, Dr. CH Yan, Dr. PK Chan, Dr. FY Ng

Professor KY Chiu, Dr. CH Yan, Dr. PK Chan, Dr. H Fu, Dr. MH Cheung

Professor KY Chiu, Dr. CH Yan, Dr. PK Chan, Dr. H Fu, Dr. MH Cheung, Dr. A Cheung, Dr. VWK Chan

Professor KY Chiu, Dr. PK Chan, Dr. H Fu, Dr. MH Cheung, Dr. A Cheung, Dr. VWK Chan, Dr. M Luk

Awards
Numerous awards have been won by members and those affiliated with the Division over the years at the Hong Kong Orthopaedic Association Annual Congress.
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Tang Wai Man
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yau Wai Pan
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Tang Wai Man
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yan Chun Hoi
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yan Chun Hoi
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yan Chun Hoi
- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yan Chun Hoi - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Chan Wai Kwan Vincent

- Arthur Yau Award for Best Clinical Paper:
Dr. Chan Ping Keung Lewis - Best Basic Science Paper presented by a local orthopaedic surgeon:
Dr. Yan Chun Hoi - Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Ng Fu Yuen - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. So Lok Wah Noah

- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Ng Fu Yuen - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Chan Wai Kwan Vincent - Best paper presented by trainee member:
Dr. Chan Wai Kwan Vincent


- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Yan Chun Hoi - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Chan Wai Kwan Vincent - Arthur Yau Award for Best Clinical Paper:
Dr. Chan Wai Kwan Vincent - Best Basic Science Paper presented by an associate member:
Zhang Chaofan


- Dr. Yeung Sai Hung Trophy for best oral paper on adult joint reconstruction by an associate member:
Chen Kam Wai - AR Hodgson Award for Best Clinical Paper:
Dr. Amy Cheung - Arthur Yau Award for Best Clinical Paper:
Dr. Henry Fu


- Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Chan Ping Keung Lewis - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Fok Chi Him Kevin - Best paper presented by trainee member:
Dr. Fok Chi Him Kevin


- Arthur Yau Award for Best Clinical Paper:
Dr. Amy Cheung - Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Amy Cheung - Dr. Yeung Sai Hung Trophy for best oral paper on adult joint reconstruction by an associate member:
Chen Hong Tai


- AR Hodgson Award for Best Clinical Paper:
Dr. Amy Cheung - Arthur Yau Award for Best Clinical Paper:
Dr. Chan Ping Keung Lewis - Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Chan Ping Keung Lewis - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Brian Lik Hang Leung - Dr. Yeung Sai Hung Trophy for best oral paper on adult joint reconstruction by an associate member:
Thomas Chak Ming Tang

- AR Hodgson Award for Best Clinical Paper:
Dr. Cheung Man Hong - Dr. David Fang Trophy for best paper on adult joint reconstruction by a local fellow:
Dr. Amy Cheung - Dr. Vincent Chan Trophy for best oral paper on adult joint reconstruction by a local orthopaedic trainee:
Dr. Samuel Fang

